Chest infections
Chest infections (sometimes called chest exacerbations) occur when bugs (bacteria or viruses) start growing in the mucous of the airways. To try and get rid of the infection, the lungs make more mucous, and the combination of more mucous and the irritation caused by the infection causes coughing. Without treatment infections can go on for several days and sometimes weeks. It is these long infections that slowly damage the lung.
How do I know when a chest infection has started?
Cough is the most important symptom. All children get normal coughs and colds, but if the cough has been going on for more than 3 days in a row, particularly if the cough sounds rattly, then we would call that a chest infection and recommend that a 2 week course of antibiotics is started. Ideally we would take a cough swab or sputum sample, but sometimes this is not practical. Usually children do not feel unwell when they have a chest infection, and will not have a fever. If they see a doctor, the doctor may say that the chest 'sounds clear'. This DOES NOT mean that there isn't a chest infection if children with CF are coughing, they need to be on antibiotics. If we do collect a cough swab or sputum sample, and that sample does not grow any bugs, this DOES NOT mean that there isn't a chest infection it just means that we have failed to grow the bug. If children with CF are coughing, they need to be on antibiotics.
Sometimes infections can be present in the airway mucous without causing any symptoms. We know that these infections can still be causing airway irritation and so need to be treated. This is why we collect cough swabs and sputum samples at every routine clinic visit and treat all infections that are found.
What if the first course of antibiotics do not work?
If after 2 weeks of antibiotics the cough has not gone away, you need to contact your local CF team and ask them for advice. Sometimes, depending on the severity of the cough, we will want to see children at this point, and collect another cough swab or sputum sample. If children are well and the cough is not severe we will often change the antibiotics and give a further 2 week course. If they are unwell, or they are still coughing after the second 2 weeks of antibiotics, they will most likely need a course of intravenous antibiotics. Giving the antibiotics directly into a vein gives a much higher concentration of the antibiotics in the lungs, and so is more effective at killing the bacteria.
Intravenous antibiotics
When chest infections do not clear up using oral antibiotics, we need to use intravenous antibiotics (often called 'ivs'). This allows a higher concentration of the antibiotic to get to the lung and so is more effective at killing the bacteria. A course of ivs is usually 2 weeks, but can be longer. Using ivs is part of routine care - about 6 out of 10 children with CF will need at least one course of ivs each year. Like all the other treatments we use, the idea is to keep children as well as possible, rather than waiting until they are unwell before starting treatment.
Intravenous access
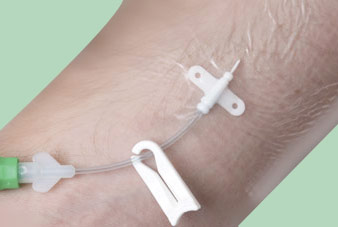 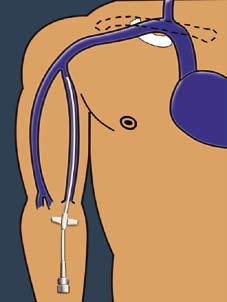 Mid-lines Mid-lines
For most children, intravenous antibiotics go into a vein through a thin plastic tube called a 'mid-line', which is usually sited in the crook of the elbow. These lines stay in for the duration of the ivs (usually 2 weeks). Sometimes the lines last the whole 2 weeks, sometimes they get blocked and need to be replaced. They are taken out at the end of the iv course.
 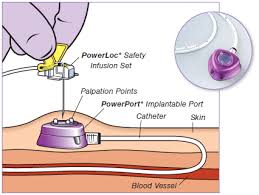 Port-a-cathSome children who need frequent ivs will have a permanent indwelling device called a 'port-a-cath'. These devices need to be inserted at an operation using general anaesthesia. They have the benefit of providing ready and easy access to the veins, and can often be used to take blood. Their disadvantage is that the need to be flushed once per month. Ports usually last 5-7 years, and can only be replaced a few times, so we don't put them in unless we have to (usually because we either can't get midlines in, or they are lasting only a few days each time). Port-a-cathSome children who need frequent ivs will have a permanent indwelling device called a 'port-a-cath'. These devices need to be inserted at an operation using general anaesthesia. They have the benefit of providing ready and easy access to the veins, and can often be used to take blood. Their disadvantage is that the need to be flushed once per month. Ports usually last 5-7 years, and can only be replaced a few times, so we don't put them in unless we have to (usually because we either can't get midlines in, or they are lasting only a few days each time).
Hospital or home?
If a child has had ivs before and their parents have had the necessary training, ivs can be given at home. We use a home delivery service (currently provided by BUPA) to deliver the ivs to the family home.
School age children can often carry on going to school during this period. The first course of ivs will usually mean being in hospital for 2 weeks. Hospital admissions can also be a good time to have an update on all aspects of CF care, including diet and physiotherapy.
| 




